Disaster Triage, Prioritizing, and Delegation
4 Topics | 2 Quizzes
Neurological System
10 Topics | 1 Quiz
MS, MG, and Guillain Barré
4 Topics | 1 Quiz
The Cardiovascular System
12 Topics | 1 Quiz
Pulmonary System
10 Topics | 1 Quiz
Cushing Versus Addison Disease
3 Topics | 1 Quiz
Thyroid Disorders
2 Topics | 1 Quiz
Parathyroid Disorders
3 Topics | 1 Quiz
DI and SIADH
3 Topics | 1 Quiz
Diabetes
10 Topics | 1 Quiz
Burns
5 Topics | 1 Quiz
Anemias, Aplastic Anemia, Polycythemia Vera, Thrombocytopenia and DIC
9 Topics | 1 Quiz
Cancer, Chemotherapy, Radiation Therapy, and Oncological Emergencies
6 Topics | 1 Quiz
Leukemias, Hodgkin’s Disease, and Multiple Myeloma
4 Topics | 1 Quiz
The GI system
16 Topics | 1 Quiz
Renal and Genitourinary Problems
6 Topics | 1 Quiz
Infection and Isolation Precautions
3 Topics | 1 Quiz
NCLEX Pharmacology
3 Topics | 1 Quiz
TPN, IV Solutions, & Blood Products
6 Topics | 1 Quiz
Lab Values
9 Topics
Pacemakers
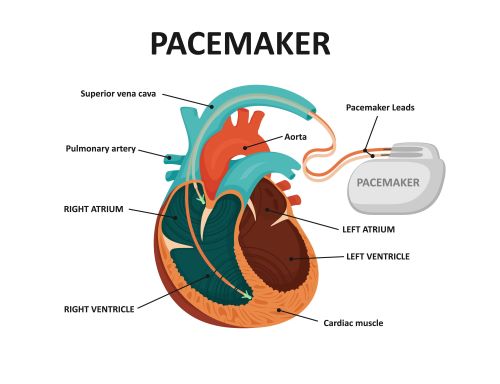
- Pacemakers are electronic devices that deliver controlled electrical stimuli to the heart muscle to regulate its rhythm.
- Pacemaker-related complications can include infection at the surgical site, lead dislodgement, pneumothorax, embolism, malfunction or electrical issues, or interference with other devices.
Assessment
- Decreased heart rate or a heart rate below the set rate means that the pacemaker is malfunctioning.
- There is a problem if the client’s heart rate is 55 and the pacemaker low rate is set at 60.
- Symptoms of decreased cardiac output such as decreased LOC, dizziness, chest pain, shortness of breath, diaphoresis, nausea and vomiting means that the pacemaker is not working.
- At the hospital, monitor EKG for inappropriate sensing and pacing.
- Monitor for dysrhythmias
Client Teaching: NCLEX Alert
- Teach the client to check his pulse every day and notify the physician of any changes.
- Teach the client to avoid excessive bending, stretching, heavy lifting, strenuous exercise or contact sports for about 8 weeks post pacemaker placement. Excessive activity may cause lead dislodgment.
- Teach the client to limit arm activity. Raising the arm above shoulder level may cause lead dislodgement. That is, do not raise arm above shoulder level.
- Teach the client to avoid shoulder-strap purses, suspenders, or firing rifles resting over the generator site.
- Instruct the client to wear a Medic Alert Bracelet with information about the type and rate of the pacemaker.
- Instruct the client to avoid electromagnetic fields and MRI.
- Televisions, electric blankets, toasters, microwave ovens, heating pads, radios, and hair dryers are considered safe.
- NOT SAFE are: devices with strong magnetic fields such as anti-theft devices at stores, metal detectors at airports, and radiation therapy.
- Instruct the client to notify the physician if he or she experiences dizziness or palpitations.
Pacing
- When the pacer paces, it creates a pacer spike.
- For atrial pacing, you will see a spike at the beginning of the P wave.
- For Ventricular pacing, you will see a spike at the beginning of the QRS complex.
- For AV pacing, you will see both an atrial spike and a ventricular spike.
- If the spike is followed by either a P wave or a QRS (depending on whether we are pacing the atria or the ventricles) then we say that the pacemaker is “capturing.” It is doing what it is supposed to do.
- If you see a spike on the EKG monitor and no P wave or QRS, then the pacemaker is not capturing. It is not creating a pulse or it is not creating the electrical activity for the heart to contract. Dangerous!
Ventricular Pacing
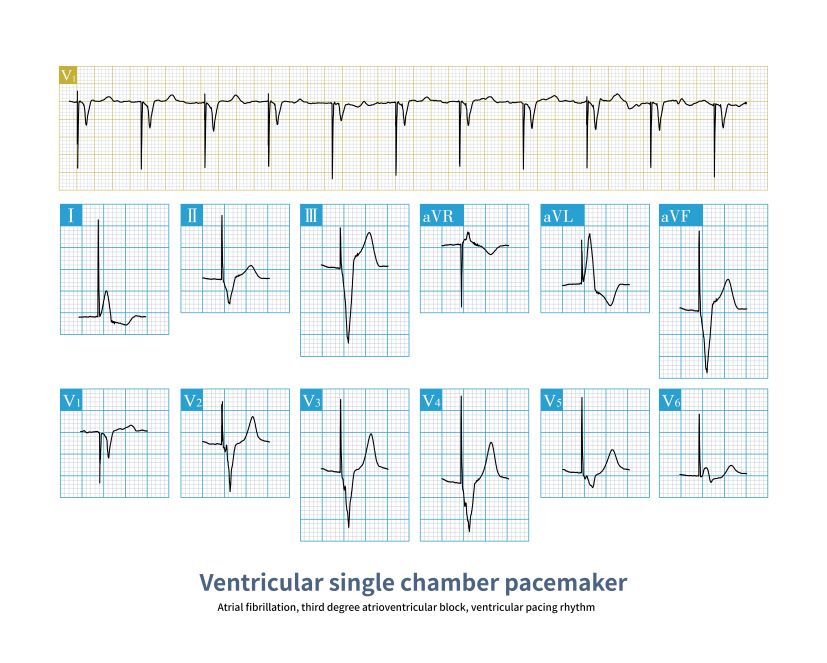
AV Pacing
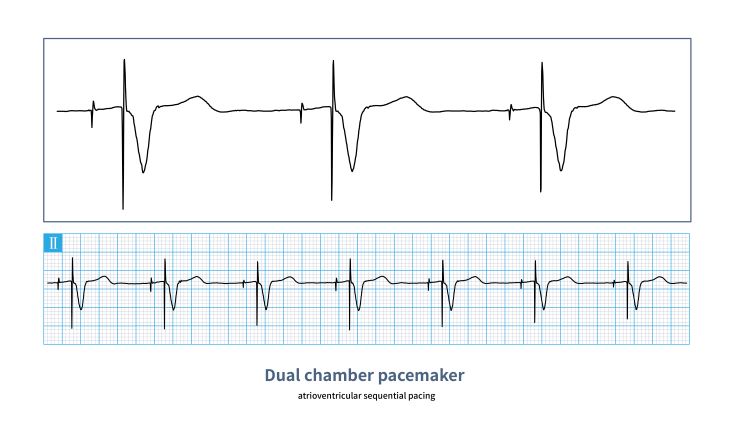
Sensing
Sensing means that if the pacer senses that the client has his or her own P wave or QRS complex, it will not fire. If the pacemaker fires, the client can go into dysrhythmias.
Examples
Here is a dangerous “failure to capture” malfunction of the pacemaker. Notice the paced beats at the beginning and the end. That’s when the pacemaker is working. When the pacemaker is not working, there is no QRS or ventricular contraction. No pulse. The client’s underlying rhythm might as well be asystole since a little atrial contraction (or P waves) is worthless.
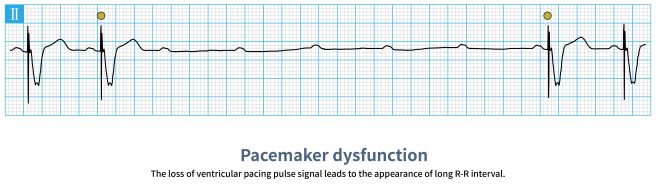
The one below is not as bad. At least the client has more paced beats or a more life-producing rhythm.